Multidisciplinary team decision is rare and decreasing in percutaneous vascular interventions despite positive impact on in-hospital outcomes
Abstract
Abstract.Background: Worldwide prevalence of peripheral artery disease (PAD) is increasing and peripheral vascular intervention (PVI) has become the primary invasive treatment. There is evidence that multidisciplinary team decision-making (MTD) has an impact on in-hospital outcomes. This study aims to depict practice patterns and time changes regarding MTD of different medical specialties. Methods: This is a retrospective cross-sectional study design. 20,748 invasive, percutaneous PVI of PAD conducted in the metropolitan area of Hamburg (Germany) were consecutively collected between January 2004 and December 2014. Results: MTD prior to PVI was associated with lower odds of early unsuccessful termination of the procedures (Odds Ratio 0.662, p < 0.001). The proportion of MTD decreased over the study period (30.9 % until 2009 vs. 16.6 % from 2010, p < 0.001) while rates of critical limb-threatening ischemia (34.5 % vs. 42.1 %), patients´ age (70 vs. 72 years), PVI below-the-knee (BTK) (13.2 % vs. 22.4 %), and rates of severe TASC C/D lesions BTK (43.2 % vs. 54.2 %) increased (all p < 0.001). Utilization of MTD was different between medical specialties with lowest frequency in procedures performed by internists when compared to other medical specialties (7.1 % vs. 25.7 %, p < 0.001). Conclusions: MTD prior to PVI is associated with technical success of the procedure. Nonetheless, rates of MTD prior to PVI are decreasing during the study period. Future studies should address the impact of multidisciplinary vascular teams on long-term outcomes.
Introduction
Peripheral artery disease (PAD) has become a global problem with significant impact on national healthcare systems. Over the past years, the prevalence of PAD has augmented in many countries. A recent systematic review estimated approximately 202 million people living with PAD worldwide [1]. Peripheral vascular interventions (PVI) for critical limb-threatening ischemia (CLTI), increased by 46 % from 2005 to 2009 in Germany [2, 3] and the German Federal Statistics Bureau reported an increasing number of procedures with more than 300,000 PVIs for PAD in 2015 [4]. In a recently published study, we reported an association of multidisciplinary team decision-making (MTD) and radiation dose for percutaneous PVIs conducted by various medical specialties [5]. MTD is recommended by international guidelines especially in the treatment of intermittent claudication (IC) due to the paucity of conclusive evidence [6–10]. However, no consensus exists regarding the definition of a multidisciplinary vascular team in PAD treatment. MTD has been found to be associated with improved clinical outcomes and alterations in treatment recommendations in the oncological field [11–13]. This study aims to describe practice patterns and time trends of MTD in patients with PAD treated by PVI, employing data from a large prospective, population-based, multicentre, quality improvement registry in the metropolitan area of Hamburg, Germany, and to evaluate the association of MTD with technical success rate and in-hospital outcome.
Methods
The statutory quality improvement registry (EQS registry) for PAD in the metropolitan area of Hamburg, Germany was introduced in 2004 and registers prospectively all percutaneous PVI performed for PAD. This study is a retrospective cross-sectional study of procedures conducted between January, 2004 and December, 2014. The study time period was chosen in regard of the implementation of the registry in 2004 and a major revision of data definitions in 2015. The parameters collected by the EQS registry were defined a priori as a consensus by experts in 2004, with minor revisions in 2008. This EQS registry includes all inpatient procedures conducted at legally endorsed privately or publicly owned hospitals within the metropolitan region of Hamburg in Germany (approximately 1.8 million inhabitants in Hamburg and 5.3 million inhabitants in the extended metropolitan region) (ESM 1). The number of participating centres varied from 12 in 2004, to 17 in 2014 (overall 20 different centres performed PVIs during the study period). Each participating centre includes access to departments for vascular surgery, radiology, and internal medicine. No hub and spoke model was deployed in the metropolitan area of Hamburg. Exclusion criteria were open surgery or hybrid cases and solely diagnostic angiographies without peripheral arterial revascularization. An external and internal validation is performed annually by random sample matching and cross-checking with hospital diagnosis data from the German Federal Bureau of Statistics. External validity was reported to be 91.8 % to 99.1 % from 2010 to 2014 [5]. For this study, we utilized information on patient age, gender, medical specialty of the interventionalist, indication for the procedure, revascularization (procedure) of crural vessels below-the-knee (BTK) performed, TASC-classes C or D indicating high lesion severity, disease severity score, MTD, treadmill test conducted, admission date, procedure date, early unsuccessful termination of the procedure, discharge date, overall and postoperative length of stay, postprocedural complications, and discharge destination. Indication for the procedure was collected by Rutherford classification for chronic limb ischemia (category 0 for asymptomatic PAD, categories 1 to 3 for intermittent claudication, category 4 for ischemic rest pain, categories 5 to 6 for tissue loss). Unless otherwise indicated, categories 1 to 3 were pooled to IC, categories 4 to 6 were pooled to CLTI. The disease severity score was calculated as a summation of TASC-classes as defined by the Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II) [14] from TASC A (1 point) to TASC D (4 points). Evaluations of all lesions in aorto-iliac, femoropopliteal, and crural vessels evaluated by angiography were used as summands (0 to 12 points per leg). No follow-up data were collected after hospital discharge. Postprocedural complications include occlusion, pseudoaneurysm, revision due to major bleeding, dissection, embolism, other complication (includes amputation, no further specification of complications) and in-hospital mortality. The procedures conducted by internists, angiologists, and cardiologists are merged into one discipline: internal medicine. Early unsuccessful termination of the procedure, considered as incomplete revascularization, was stated if the procedure were aborted before the arterial revascularization was successful.
Multidisciplinary team decision
The EQS-registry includes the question whether the index procedure had been previously discussed and settled between different medical specialties (vascular surgery, radiology, internal medicine). The different vascular specialists attending the case discussion and reconciliation were submitted in detail. MTD was stated if the PVI were based on a prior case discussion following the abovementioned criteria with all three vascular medical specialties attending the meeting. Multidisciplinary case discussions with only two of three specialists attending were not stated as MTD.
Ethical considerations
Informed consent of the submission of anonymized data to the EQS registry was obtained for all cases. Since EQS is a regulatory statutory, quality improvement project of the Hamburg government, the analysis of anonymized registry data could be executed without objections by the local ethics committee.
Statistical analysis
Depending on the distribution, data are presented either with mean and standard deviations (SD) or with median and interquartile ranges (IQR) for continuous variables. Proportions are reported by percentages and 95 % confidence interval (CI). Bootstrapping was used to estimate the accuracy of given estimators such as standard errors and confidence intervals. Tests of normality were conducted by the Kolmogorov-Smirnov test while the Mann-Whitney U and Kruskal-Wallis H tests were used for comparison of abnormally distributed data. Rates were compared with Fisher´s exact test of independence or Chi-square test. An adjusted logistic regression approach was conducted to investigate the impact of relevant covariates (age, gender, critical limb ischemia, involvement of crural vessels BTK, higher disease severity score, prior MTD) on early unsuccessful termination of the procedure. An adjusted logistic regression approach was also conducted to investigate the impact of relevant covariates (age, gender, procedure conducted by vascular surgeons, critical limb ischemia, involvement of crural vessels BTK, higher disease severity score) on the likelihood that a prior MTD had been conducted. A p-value of < 0.05 was regarded as statistically significant. Statistical analyses were performed with IBM SPSS Statistics software version 25.0 (IBM, Armonk, NY, U. S.).
Results
Patients and procedures
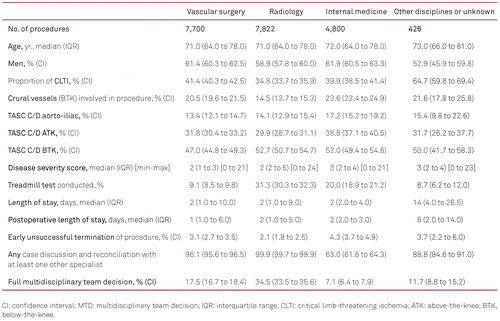
Baseline characteristics of the study population for several medical specialties performing the PVIs are given in Table I. A total of 20,748 procedures were identified. 12,444 procedures (60.8 %, CI 60.1–61.5) were conducted for IC and 7,957 procedures (38.9 %, CI 38.2–39.6) were performed for CLTI. A small proportion (1.7 %, CI 1.5–1.9) of procedures was conducted for asymptomatic PAD or unknown Rutherford category. The proportion of CLTI was 34.8 % (CI 33.7–35.9) in radiology, 39.9 % (CI 38.5–41.4) in internal medicine, and 41.4 % (CI 40.3–42.5) in vascular surgery. The proportion of TASC C/D lesions varied between anatomic regions and medical specialties (Table I). A total of 12,419 (60.5 %, CI 59.8–61.2) procedures were conducted in male patients and 8,113 (39.5 %, CI 38.8–40.2) in female patients. Median age of males was 70.0 years (IQR 62.0 to 76.0) and significantly (p < .001) lower than age of females (74.0 years, IQR 66.0 to 81.0).
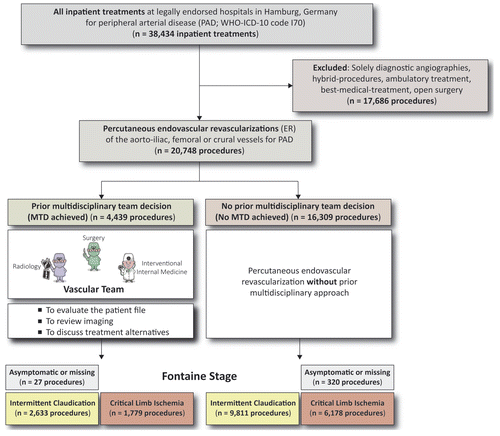
Multidisciplinary team decision-making
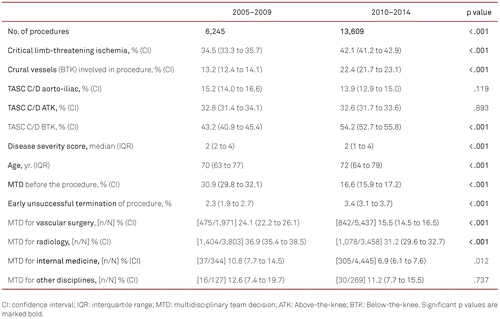
In total, 4,439 (21.4 %, CI 20.8–22.0) procedures were conducted following prior MTD (Figure 1). The overall proportion of MTD in different specialties ranged between 7.1 % (CI 6.4–7.9) for internal medicine, to 34.5 % (CI 33.5–35.6) for radiology (Table I). The proportion of procedures following MTD decreased from 2005–2009 (30.9 %, CI 29.8–32.1) to 2010–2014 (16.6 %, CI 15.9–17.2) (p < 0.001), while patient age, BTK procedure, high plaque burden BTK, and the proportion of CLTI as reason for the intervention increased over the same period (p < 0.001) (Table II). The rate of MTD diminished from 2005–2009 to 2010–2014 for all medical specialties (Table II).
Predictors on prior multidisciplinary team decision
A multivariate logistic regression was performed to ascertain the effects of higher age (increase per one year), female gender (vs. male gender), occurrence of CLTI (vs. IC), internal medicine performing the procedure, BTK procedure, and higher disease severity score (increase per one TASC-classification) on the likelihood that a prior MTD (including all three medical specialties) had been conducted. All covariates added significantly to the model (results not shown in tables). BTK procedure (OR 1.356, CI 1.234–1.489, p < .001) and higher plaque burden (OR 1.222, CI 1.207–1.236, p < .001) were associated with higher odds of prior full MTD. Higher age (OR 0.993, CI 0.989–0.996, p<.001), female gender (OR 0.906, CI 0.841–0.976, p = .009), occurrence of CLTI (OR 0.850, CI 0.784–0.921, p < .001), and internal medical specialty of the operator (OR 0.304, CI 0.269–0.343, p < .001) were associated with lower odds of prior MTD (results not shown in tables).
Unadjusted outcomes following MTD by IC vs. CLTI
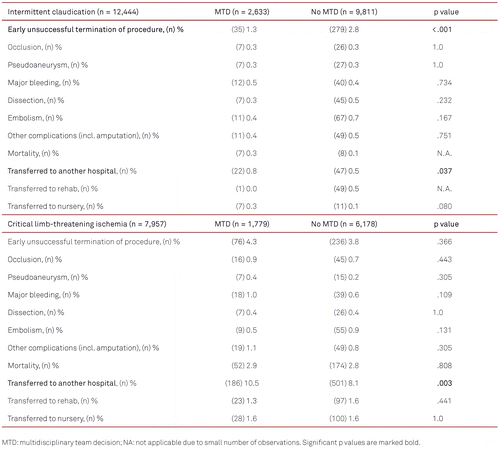
Outcome parameters stratified for IC and CLTI are given in Table III. If MTD were made, the early unsuccessful termination rate was lower (2.5 % vs. 3.2 %, p=0.019, results not shown in tables), reaching statistical significance for treatment of IC (1.3 % vs. 2.8 %, p < 0.001), but not for treatment of CLTI (4.3 % vs. 3.8 %, p = .366). The patients were more often transferred to another hospital if MTD were made pre-interventional in the IC-group (0.8 % vs. 0.5 %, p = .037) and in the CLTI-group (10.5 % vs. 8.1 %, p = .003). Due to the small number of events, valid p values could not be calculated for all group differences.
Predictors on early unsuccessful termination of the procedure
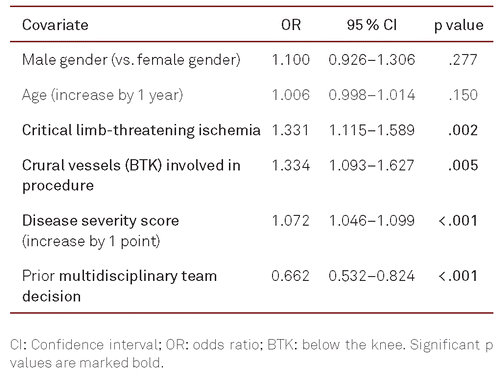
A multivariate logistic regression was performed to ascertain the effects of higher age, male gender, occurrence of CLTI, BTK procedure, disease severity score (increase per one TASC-classification), and prior MTD (including all specialists) on the likelihood that the procedure was unsuccessfully terminated early. Regression coefficients and confidence intervals can be found in Table IV. Four covariates added significantly to the model. Occurrence of CLTI (OR 1.331, CI 1.115–1.589, p = .002), BTK procedure (OR 1.334, CI 1.093–1.627, p = .005), and higher disease severity score (OR 1.072, CI 1.046–1.099, p < .001) were associated with higher odds of early unsuccessful termination of the procedure. Previous MTD (OR 0.662, CI 0.532–0.824, p < .001) was associated with lower odds of early unsuccessful termination of the procedure.
Discussion
In this first German investigation of MTD in 20,748 PVIs for PAD conducted between 2004 and 2014, using a large population-based registry, we found that MTD prior to PVI is associated with lower early unsuccessful termination rates of the procedures. While patient age, BTK procedure, high rate of TASC C/D lesions BTK, and proportion of CLTI as indication for treatment was increasing over time, utilization of MTD prior to PVI decreased. Lower MTD-rates were found in procedures conducted by internal medicine compared to other medical specialties.
Although, nearly all practical guidelines on PAD treatment recommend multidisciplinary approaches in the evaluation and treatment of this patient group, very limited evidence is available on the impact of MTD utilization [6–10]. Furthermore, a clear definition of MTD is lacking. The recently published 2017 European Society of Cardiology (ESC) guidelines on the Diagnosis and Treatment of PAD, in collaboration with the European Society for Vascular Surgery (ESVS), recommend a multidisciplinary Vascular Team to form decisions for the management of patients with PADs (Class I, Level C), emphasizing the need for multidisciplinary management of these patients [9].
Suzuki et al. recently illuminated the efficacy of a multidisciplinary team approach in 145 patients suffering from Fontaine stage IV in a prospective single centre study. The authors found significantly improved outcomes if the patients were treated by a multidisciplinary care team [15]. Chung et al. conducted a retrospective single-centre study of 146 consecutive CLTI patients, targeting the impact of multidisciplinary care on amputation-free survival (AFS). The authors revealed a two-fold increase in AFS in patients treated by a multidisciplinary care team [16]. Hioki et al. retrospectively analysed 72 patients with CLTI and assessed whether multidisciplinary therapy improved prognosis. An improved mortality and limb salvage rate were identified if the treatment were conducted under multidisciplinary conditions [17]. Zayed et al. investigated the impact of multidisciplinary approach on the major amputation rates in diabetic patients with CLTI. The authors retrospectively included 312 patients and found improved outcomes following MTD [18]. These few abovementioned studies are limited by small study size. Furthermore, the impact of MTD on procedures conducted for IC remains unclear. Nevertheless, our study can confirm the overall positive impact of MTD on technical success of the procedure.
The association between prior MTD and lower early unsuccessful termination rates might be explained by the fact that sharing multidisciplinary experiences may lead to lower numbers of patients considered suitable for PVI. In the present study, the rates of early unsuccessful terminations were lower for vascular surgery compared to internal medicine (3.1 % vs. 4.3 %), potentially attributable to higher rates of pre-interventional MTD in vascular surgery compared to internists (17.5 vs. 7.1 %, Table I), or to a lower rate of BTK lesions. The significantly lower rate of severe TASC C/D lesions BTK in procedures performed by vascular surgery when compared to internal medicine confirms the likely difference in patient selection. To which degree the aggressiveness of endovascular attempts might be impacted by available alternative approaches (e. g. lower extremity bypass) remains ill-defined. Furthermore, a more aggressive endovascular approach in a population with increasingly complex lesions may lead to higher technical success rates. In contrast to this observation, the rates of treadmill testing prior to the procedures were lower for vascular surgeons (9.1 %), compared to radiologists (31.3 %) or internists (20.0 %). A significant inverse relation between increasing patient age, rate of BTK procedures, and proportion of CLTI on the one hand and decreasing MTD on the other hand was noticed over the study period. Since especially complex cases (reflected by CLTI, procedures involving crural vessels with high TASC classes, and higher disease severity score) deserve a multidisciplinary approach, this trend appears interesting. Notably, a statistically significant association of prior MTD and early unsuccessful termination in procedures could be noticed only in patients with IC but not in patients with CLTI. This observation might be explained by several reasons. Patients suffering from CLTI are more frequently treated BTK when compared to IC [5, 19, 20] and it seems possible that these more pretentious lesions are primarily treated by well-experienced operators when compared to lesions ATK, leading to overall lower early termination rates. Another possible explanation might be that interventionalists perform procedures for CLTI with particular emphasis to avoid amputations while procedures performed for IC primarily aim to improve the disease-related quality of life. Unfortunately, this study cannot validly answer this question. MTD plays an important role in various health-care disciplines, especially considered standard in multimodal cancer therapy [13]. Studies have shown a superiority in success rates and survival when MTD had been conducted prior to surgical cancer treatment [12, 20, 21]. These encouraging results may partly be evident in other medical specialties as multidisciplinary care teams are associated with lower mortality on intensive care units [22]. Furthermore, a large systematic review including 29 randomized controlled trials, assessing the effects of MTD in cardiology, concludes reduced rates of hospitalisation with heart failure and an overall decrease in all-cause mortality [23]. Accordingly, the concept of cardiovascular Heart Teams in the management of complex cardiac diseases is recently disseminating into worldwide healthcare centres [24]. While the caseload of PVI for PAD [1, 2] increases, it appears interesting that MDT utilization decreases despite accepted benefits and guideline recommendations.
The vascular team in PAD treatment
We recommend implementing regular multidisciplinary meetings including at least vascular surgeons, radiologists, and internists to review existing diagnostic imaging of the patients under elective conditions.
Limitations
First, this study is limited to in-hospital outcomes without long-term follow-up and without information on patency or target limb revascularization [25]. Secondly, all analyses were based on single interventions. In Germany, it is forbidden by law to re-identify individual patients. However, only 1.2 % of all patients had more than one intervention during the index hospital stay. Thirdly, no information regarding admission mode is collected in the EQS, which was true across specialties. It is possible that there is a selection bias since a number of urgent procedures for CLTI might be conducted before a MTD could be made. Lastly, due to the lack of commonly accepted definitions for MTD practice, we limited the MTD-covariate to procedures settled by a case discussion and reconciliation between at least one vascular surgeon, one radiologist, and one internist, bearing in mind that guidelines do not provide a protocol or model for this practice nor furnish any standard setting for Vascular Teams. This direct query was consistently available over the entire study period (2004 to 2014). Nevertheless, MTD practice might slightly differ between the hospitals. However, the findings of the present study could aid in encouraging the implementation of MTD to improve patient selection and increase rates of technical success.
Conclusions
Rates of MTD prior to PVI in PAD are low and are decreasing over time in this large population-based study although being broadly recommended by practical guidelines. MTD utilization differs significantly between medical specialties performing PVI and appears to be associated with technical success. Future studies should examine the impact of MTD on long-term outcomes.
Acknowledgements
The authors are grateful to all the surgeons, radiologists, internists, and colleagues from other special disciplines who registered patients in the EQS registry. The authors are grateful to the EQS-Hamburg Federal Office for Quality Insurance for supporting this quality improvement project. The authors thank the German Stifterverband and the CORONA foundation for financial support in the organization and publication of this study. E. Sebastian Debus and Henrik C. Rieß contributed equally to this work. The authors would like to thank Ms. Priscilla Robinson for proofreading and editing.
Compliance with ethical standards
Funding: This study was partly funded by the German Stifterverband and the CORONA foundation (grant number S199/10061/2015).
Informed consent: Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
The electronic supplementary material (ESM) is available with the online version of the article at
https://doi.org/10.1024/0301-1526/a000771.
- Hospitals within the metropolitan region of Hamburg in Germany.
Literature
Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet. 2013;382:1329–40.
Recent trends in morbidity and in-hospital outcomes of in-patients with peripheral arterial disease: a nationwide population-based analysis. Eur Heart J. 2013;34:2706–14.
. Percutaneous endovascular treatment of infrainguinal PAOD: Results of the PSI register study in 74 German vascular centers. Gefasschirurgie. 2017;22(Suppl 1):17–27.
Statistisches Bundesamt DeStatis . Krankenhausdiagnosestatistik, 2014. Available at: https://www.destatis.de/DE/ZahlenFakten/GesellschaftStaat/Gesundheit/Krankenhaeuser/Methoden/Krankenhausstatistik.html (Accessed November 14, 2016).Radiation Dosage for Percutaneous PAD Treatment is Different in Cardiovascular Disciplines: Results From an Eleven Year Population Based Registry in the Metropolitan Area of Hamburg. Eur J Vasc Endovasc Surg. 2017;53:215–22.
2016 AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Journal of the American College of Cardiology. 2017;69:e71–e126.
NICE Clinical Guideline 147 . Lower limb peripheral arterial disease. Diagnosis and management. NICE Clinical Guideline 147. Available at: http://www.nice.org.uk/guidance/cg147. (Accessed November 14, 2016).Society for Vascular Surgery practice guidelines for atherosclerotic occlusive disease of the lower extremities: management of asymptomatic disease and claudication. J Vasc Surg. 2015;61(3 Suppl):2S–41S.
2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS): Document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteries Endorsed by: the European Stroke Organization (ESO) The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). Eur Heart J. 2018;39:763–816.
Editor’s Choice – 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg. 2018;55:305–368.
The impact of a multidisciplinary breast cancer center on recommendations for patient management: the University of Pennsylvania experience. Cancer. 2001;91:1231–7.
MRI identified prognostic features of tumors in distal sigmoid, rectosigmoid, and upper rectum: treatment with radiotherapy and chemotherapy. Int J Radiat Oncol Biol Phys. 2006;65:445–51.
Improving cancer control in the European Union: conclusions from the Lisbon round-table under the Portuguese EU Presidency, 2007. Eur J Cancer. 2008;44:1457–62.
. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J Vasc Surg. 2007;45(Suppl S):S5–67.
The efficacy of a multidisciplinary team approach in critical limb ischemia. Heart Vessels. 2017;32:55–60.
. Multidisciplinary care improves amputation-free survival in patients with chronic critical limb ischemia. J Vasc Surg. 2015;61:162–9.
Prognostic improvement by multidisciplinary therapy in patients with critical limb ischemia. Angiology. 2015;66:187–94.
. Improving limb salvage rate in diabetic patients with critical leg ischaemia using a multidisciplinary approach. Int J Clin Pract. 2009;63:855–8.
. Sex-Based Assessment of Patient Presentation, Lesion Characteristics, and Treatment Modalities in Patients Undergoing Peripheral Vascular Intervention. Circ Cardiovasc Interv. 2018;11:e005749.
. Population-based analysis of gender disparities in 23,715 percutaneous endovascular evascularisations in the metropolitan area of Hamburg. Eur J Vasc Endovasc Surg. 2018 [in Press].
Multidisciplinary team management is associated with improved outcomes after surgery for esophageal cancer. Dis Esophagus. 2006;19:164–71.
. The effect of multidisciplinary care teams on intensive care unit mortality. Arch Intern Med. 2010;170:369–76.
. Multidisciplinary strategies for the management of heart failure patients at high risk for admission: a systematic review of randomized trials. J Am Coll Cardiol. 2004;44:810–9.
. The heart team of cardiovascular care. J Am Coll Cardiol. 2013;61:903–7.
Indicators of outcome quality in peripheral arterial disease revascularisations – a Delphi expert consensus. Vasa. 2018;47:491–497.



