The compelling arguments for the need of medical vascular physicians in Europe
Abstract
Summary. The burden of vascular diseases is growing worldwide, as the population ages, prompting a call to action not only in terms of awareness but also and most urgently in recognizing the need for vascular physicians, also called angiologists. Vascular medicine views the vascular system (arteries, veins, and lymphatics) as a whole, unique, and independent entity requiring specialized competencies. Vascular physicians offer a holistic and comprehensive approach to vascular patients including provision of interventional procedures, management of a heterogeneous group of multi-morbid and frail patients affected by multi-vessel diseases, and connecting different specialists in a multidisciplinary effort. Vascular medicine practise varies across European countries. While it is a firmly accepted medical speciality in many European countries it is not formally recognized by the European Union limiting adoption in the other countries. The lack of vascular physicians likely accounts for inequality of care of vascular patients as compared for example to patients with heart disease and might contribute to adverse outcomes and healthcare costs associated with vascular diseases. To move forward in the struggle to provide efficient care for multimorbid poly-vascular patients, it is essential to establish vascular medicine programs in Europe and worldwide. Important steps to achieve this goal include improving public awareness of vascular diseases, attain formal recognition by the EU of angiology/vascular medicine as a medical specialty, creating specialized treatment guidelines, and to harmonize vascular care in Europe.
Introduction
Vascular diseases affecting arteries, veins, lymphatics, and the microcirculation represent a large and growing health burden throughout Europe. It is estimated that peripheral artery disease (PAD) may affect more than 20 % of elderly people worldwide [1, 2] while venous thromboembolism accounts for an incidence of 104–183 per 100,000 person years (similar to stroke) [3]. Further, one out of three suffers from venous insufficiency, and approximately 140 to 250 million people worldwide have lymphedema, which is still largely underestimated. The burden of vascular diseases is estimated to grow worldwide, as the population ages, prompting a call to action not only in terms of awareness but also and most urgently in recognizing the need for vascular physicians, also called angiologists. In order to offer a holistic and comprehensive approach to vascular patients, vascular physicians need to be able to manage a heterogeneous group of multi-morbid and frail patients affected by multi-vessel diseases, and to connect different specialists including vascular surgeons, radiologists, cardiologists, dermatologists, and diabetologists in a multidisciplinary effort. There is a compelling medical need to avoid further fragmentation and inequality of care, in vascular patient management, which has been so frequently documented [4, 5]. This fragmentation is somewhat historically based on differing national and even local practices, as a result of the inability of other specialties to view the vascular system (arteries, veins, and lymphatics) as a whole, unique, and independent organ requiring specialized competencies [6, 7]. Recognizing the need to federate vascular physicians and raise awareness on vascular diseases, the European Society for Vascular Medicine (ESVM) was created in 2012 bringing under the same umbrella vascular physicians throughout Europe [8]. In several countries vascular medical specialists are already established as a discipline within internal medicine. In many European countries they are called angiologists, and there the medical specialty is referred to as angiology (from the Greek word angios meaning vessel and logos meaning study). Globally, however, they are mostly called vascular physicians, and the medical speciality is vascular medicine. While angiology and vascular medicine are synonyms [9], this difference in terminology contributes to a dispersion of unifying vision and creates a certain confusion within the health care community as well as within the population at large limiting visibility of this speciality. This issue needs to be addressed at the European level.
Variability of vascular medicine practice throughout Europe
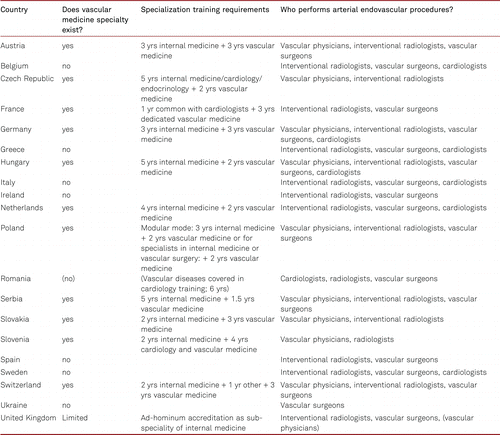
Currently, the way patients with (multiple) vascular diseases are managed is quite heterogeneous in Europe and dispersed across multiple specialties. Vascular medicine aims at integrating the care for the vascular system as a whole and connecting the different professionals. Besides vascular physicians, vascular surgeons, cardiologists, interventional radiologists, diabetologists, rheumatologists, neurologists, and dermatologists play important roles in the management of vascular patients, as do professions allied to medicine such as podiatrists, physiotherapists, vascular nurses, and technologists. Depending on the country, and even on local institutions, the role and contribution of each specialty to the management of vascular patients vary widely (Table I). While in central Europe’s countries, vascular physicians (deriving from internal medicine) play a major role, in many others the vascular field is dominated, or even monopolized, by general or vascular surgery. In these central European countries, vascular physicians also participate in the provision of effective endovascular treatment of peripheral artery disease and progressively venous disease (Table I). The development of vascular medicine is often hampered by natural competition with other specialities, mainly in the area of endovascular therapy. The lack of recognition of one vascular medicine specialty managing vascular patients and coordinating the multidisciplinary effort likely accounts for inequality of care of vascular patients as compared for example to patients with heart diseases and possibly contributes to high rates of adverse events and healthcare costs associated with vascular diseases.
The need for medical vascular physicians
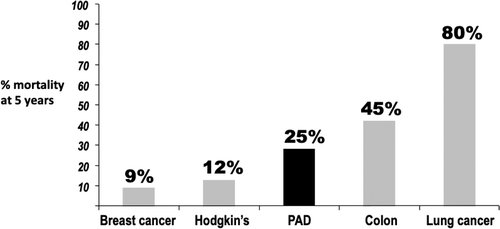
The burden of aging multimorbid patients with several significant vascular problems is rising worldwide [2]. German secondary care data on PAD patients exemplify this showing that prognosis of many vascular patients is as bad as that of patients with Duke’s stage 2b colon cancer [10]. Almost half of the patients undergoing amputations did not receive any vascular diagnostics within 2 years prior to amputation and amputation accounts for a significant proportion of healthcare costs [11, 12]. The situation is similar, and may be even worse, in other countries. Overall, mortality of PAD patients at 5 years is high and exceeds that of some common cancers (Figure 1).
Further compared to coronary disease, the sub-optimal management of vascular risk in these patients is well documented, resulting in an unacceptably high incidence of myocardial infarction, stroke, and cardiovascular (CV) death [13]. The REACH Registry [14] clearly linked CV endpoints to poor risk management in these PAD patients, and even within this past 12 months publications show disproportionate levels of fatal and non-fatal CV events in our patients [14, 15]. Proper diagnostics, medical, and interventional treatments as well as follow up, are a priority not only for PAD patients, but also for patients affected by venous, lymphatic, and microvascular disorders. Only a multidisciplinary approach with a strong medical basis can address the problem. Thus, medical vascular physicians are needed to face the medical need and connect specialties, to take care of chronic disease, thus filling an important gap. However, the visibility of vascular medicine amongst the general public and also among medical professionals is low.
Vascular medicine as a medical specialty in Europe
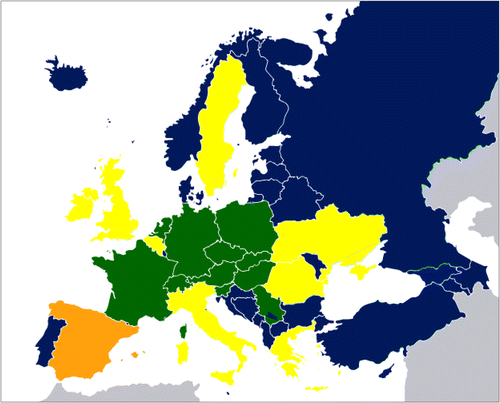
The process for the European Union (EU) to include vascular medicine as a main specialty with automatic recognition of doctor’s qualifications in all EU countries requires recognition of the speciality in at least 2/5th of the member states (article 25). While cardiology and vascular surgery exist as medical specialties in all 28 and 25 EU countries, respectively, vascular medicine is only accepted or formally accredited by medical boards of 9 EU countries. Therefore, vascular medicine is not listed as an individual specialty in the EU document [16]. However, vascular medicine is a firmly accepted medical speciality in 11 European countries, including Switzerland and Serbia. In addition, ad hominem accreditation exists in the United Kingdom and vascular medicine is taught and practised within other specialities e.g. in cardiology in Romania and Luxemburg (Table I and Figure 2). The consequence of the lack of EU recognition is inequality in patient care across Europe, failure in recognizing vascular diseases as an independent health burden, inability to set up comprehensive European programs of awareness and prevention of vascular diseases, and increase of health costs throughout Europe. Another consequence is the lack of so called “automatic recognition” process allowing vascular physicians to obtain a medical license in one country based on their training and practice as such in other countries. This seriously restricts mobility of vascular physicians across Europe thereby denying patients optimal care. The EU process permits 2 ways to include a “new” specialty onto the EU directive: (a) a specialty has to be accepted in more than 2/5th of EU countries, or (b) a compelling case of specialty need, not covered by existing ones, has to be demonstrated. In addition to the compelling medical need, the essential formal requirements to integrate vascular medicine in the EU directive requires coordination and set up of minimal training standards. Importantly, these training standards were recently developed by the Division of Vascular Medicine of the Union Européenne des Médecins Spécialistes (UEMS, European Union of Medical Specialists) [9], and ESVM (vascular-medicine.org) for diagnostic and non-invasive angiology training, and interventional therapy, respectively. Furthermore, standards and accreditation of European training centres are also being organized and vascular physicians may obtain a European Diploma of Vascular Medicine [9]. These standards can already be adopted in countries without formal recognition of vascular medicine aiming at improving inequality in care for patients with vascular disease.
The way forward
To move forward in the struggle to deal with multimorbid poly-vascular patients, it is essential to establish medical vascular medicine programs in Europe and worldwide. Additionally, key steps include improving public awareness of vascular diseases, and increasing the visibility of the importance of integrated vascular care of our patients. To achieve this goal, it is of utmost importance to attain formal recognition by the EU of angiology/vascular medicine as a specialty by presenting a compelling case and creating specialized treatment guidelines (e.g. [6]). We believe these fundamental steps will encourage most European countries to recognize vascular medicine as a specialty and will prompt other specialties to join efforts in developing vascular awareness and management not only in Europe but worldwide. Through this ‘position paper’ we hope to draw attention to the plight of the vascular patient and ask for support in our endeavours to improve their care.
ESVM board authors
Vinko Boc (Department of Vascular Diseases, University Clinical Centre, Ljubljana, Slovenia), Caitriona Canning (VascularMedicine, Trinity College and James’s Hospital, Dublin, Ireland), Patrick H Carpentier (Department of Vascular Medicine, Grenoble-Alpes University Hospital, Grenoble, France), Ali Chraim (Department of Vascular Surgery, Cedrus Vein and Vascular Clinic, Lviv Hospital, Lviv, Ukraine), Evangelos Dimakakos (Vascular Unit, 3rd Internal Medicine department, General Hospital, University of Athens School of Sotiria, Athens, Greece), Anders Gottsäter (Lund University, Department of Vascular Diseases, Skåne University Hospital, Sweden), Manuel Monreal (Hospital Universitari Germans Trias i Pujol, Badalona, Spain), Dan Mircea Olinic (University of Medicine and Pharmacy, Emergency Hospital, Medical Clinic no. 1, Cluj-Napoca, Romania), Zsolt Pécsvárady (Vascular Center, Flor Ferenc Teaching Hospital, Kistarcsa, Hungary), Isabelle Quere (Médecine Vasculaire, Université de Montpellier, Montpellier, France), Jeanine Roeters van Lennep (Erasmus University, Department of Internal Medicine, Rotterdam, Netherlands), Karel Roztocil (Institute of Clinical and Experimental Medicine, Prague, Czech Republic), Agata Stanek (Department of Internal Diseases, Angiology and Physical Medicine, Medical University of Silesia, Bytom, Poland), Dragan Vasic (Clinical Centre of Serbia, Belgrade, Serbia), Adriana Visonà (Angiology Unit, Azienda ULSS 2 Marca Trevigiana, Castelfranco Veneto, Italy), Jean-Claude Wautrecht (Service de Pathologie Vasculaire, Hôpital Erasme, Université Libre de Bruxelles Brussels, Belgium).
References
1 High prevalence of peripheral arterial disease and co-morbidity in 6880 primary care patients: cross-sectional study. Atherosclerosis. 2004;172(1):95–105.
2 Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. The Lancet. 2013;382(9901):1329–40.
3 . Epidemiology of venous thromboembolism. Nat Rev Cardiol. 2015;12(8):464–74.
4 Critical issues in peripheral arterial disease detection and management: a call to action. Arch Intern Med. 2003;163(8):884–92.
5 A structured review of antithrombotic therapy in peripheral artery disease with a focus on revascularization: A TASC (InterSociety Consensus for the Management of Peripheral Artery Disease) initiative. Circulation. 2017;135(25):2534–55.
6 ESVM guidelines – the diagnosis and management of Raynaud’s phenomenon. Vasa. 2017;46(6):413–23.
7 Requirements for angiology/vascular medicine. Int Angiol. 2013;32(6):608–12.
8 . The birth of the European Society for Vascular Medicine (ESVM) – a new step forward in the development of vascular medicine. Vasa. 2013;42(5):315–6.
9 UEMS training requirements for angiology and vascular medicine: European standards of postgraduate medical specialist training (ETR Document). Int Angiol. 2016;35(2):217–31.
10 . Cancer Facts and Figures – 2018. 2018. Available from: https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2018/cancer-facts-and-figures-2018.pdf
11 Peripheral arterial disease and critical limb ischaemia: Still poor outcomes and lack of guideline adherence. Eur Heart J. 2015;36(15):932–8.
12 Recent trends in morbidity and in-hospital outcomes of in-patients with peripheral arterial disease: a nationwide population-based analysis. Eur Heart J. 2013;34(34):2706–14.
13 . Risk factors for suboptimal utilization of statins and antiplatelet therapy in patients undergoing revascularization for symptomatic peripheral arterial disease. Ann Vasc Surg. 2018;46:234–40.
14 Statin therapy and long-term adverse limb outcomes in patients with peripheral artery disease: insights from the REACH registry. Eur Heart J. 2014;35(41):2864–72.
15 Incidence, characteristics, and outcomes of myocardial infarction in patients with peripheral artery disease: Insights from the EUCLID trial. JAMA Cardiol. 2019;4(1):7–15.
16 , Free movement of medical doctors: the new Directive 2005/36/EC on the recognition of professional qualifications. Eur J Health Law. 2005;12(4):373–96.
17 . Ten year mortality in different peripheral arterial disease stages: A population based observational study on outcome. Eur J Vasc Endovasc Surg. 2018;55(4):529–36.



